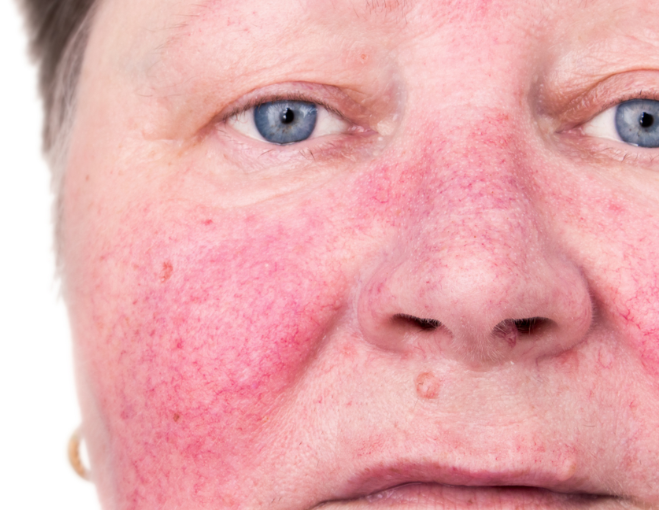
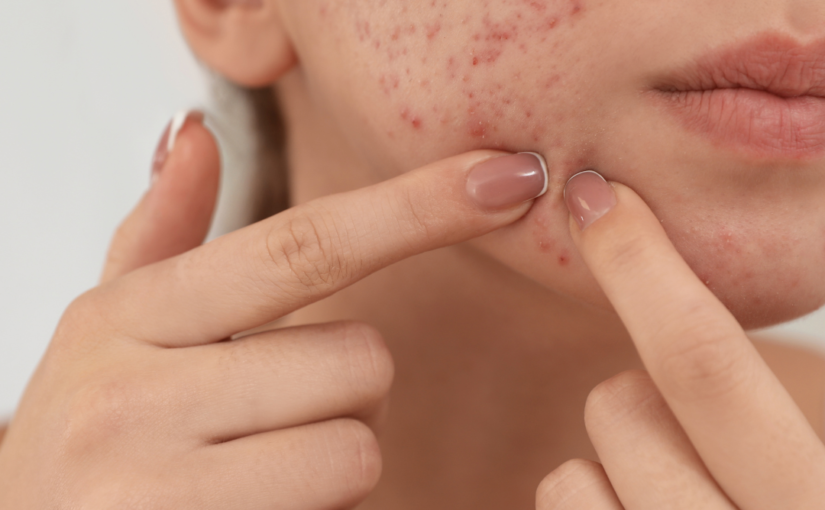
Struggling with breakouts even though you’re using what you believe is good skincare?
You’ve upgraded your cleanser. You’re using active ingredients. You’re trying to “do everything right.” And yet your skin still won’t settle.
This is one of the most common frustrations I see in clinic. People aren’t neglecting their skin. In fact, most are trying very hard. But acne is rarely about effort. It’s about understanding what your skin actually needs.
Let’s look at what might really be going on.
Acne Is More Complex Than It Looks
Acne isn’t just a blocked pore that needs drying out.
It’s a condition driven by several internal and external factors happening at the same time — oil production, inflammation, the way your skin sheds inside the pore, bacteria activity, and often hormones. If even one of those elements isn’t being managed properly, breakouts continue.
What I often see is someone treating the surface, using exfoliating acids, spot treatments, or strong cleansers, while the deeper drivers of their acne remain unaddressed.
That’s when skin gets stuck in a cycle.
When “Good” Skincare Isn’t the Right Skincare
There’s a big difference between popular products and appropriate products.
A salicylic acid cleanser may help congestion. Retinol can support cell turnover. Benzoyl peroxide can reduce bacteria. These are all useful tools.
But they’re tools, not solutions on their own.
If your acne is primarily hormonal, driven by inflammation, or linked to a compromised skin barrier, simply layering actives won’t resolve it. In some cases, it can make the skin more reactive and prolong healing.
More products doesn’t mean better results. In fact, overcomplicating a routine is one of the biggest reasons acne doesn’t improve.
The Barrier Problem No One Talks About
One of the most overlooked reasons acne lingers is barrier damage.
When you exfoliate too often, mix too many actives, or constantly switch products, the skin barrier weakens. And once that barrier is compromised, inflammation increases.
Inflamed skin produces breakouts more easily. It also takes longer to heal.
This is where the frustration builds, because you’re actively trying to treat acne, but the skin is too irritated to respond properly.
Healthy skin clears more efficiently. Angry, stripped skin does not.
Not All Acne Is the Same
Another common issue is misidentifying the type of acne you’re dealing with.
Congested acne behaves differently to inflamed, painful acne. Hormonal breakouts require a different strategy than barrier-related breakouts. Stress, lifestyle, and internal changes can all influence how acne presents.
Without a proper assessment, people often follow generic advice that doesn’t match their skin.
In clinic, once we correctly identify the type and grade of acne, progress becomes far more predictable. It’s not about trial and error. It’s about strategy.
When Skincare Alone Isn’t Enough
There’s also an important distinction between cosmetic skincare and corrective skin therapy.
Over-the-counter products can support the skin beautifully. But persistent acne sometimes requires more structured intervention, treatments that regulate cell turnover properly, reduce inflammation in a controlled way, and clear congestion at a deeper level.
This doesn’t mean your skin is “bad.” It simply means it may need more than surface-level care.
And that’s completely normal.
What I Recommend When Acne Isn’t Improving
The first step is usually to simplify.
Go back to a gentle, non-foaming cleanser. Use a barrier-supportive moisturiser. Reduce excessive exfoliation. Allow your skin to stabilise.
Then introduce targeted actives carefully and intentionally, rather than layering multiple ingredients at once.
Consistency matters more than intensity. Acne does not clear in two weeks. True change typically takes at least six to twelve weeks of the right approach.
If breakouts are persistent, painful, or starting to scar, that’s when professional guidance becomes especially important. The longer acne is left unmanaged, the more difficult it can be to treat.
A Final Thought
If your acne isn’t clearing, it doesn’t mean you’re failing. It doesn’t mean your skin is “difficult.”
It usually means the root cause hasn’t been properly assessed.
Acne is one of the most treatable skin conditions when approached correctly. With the right diagnosis, the right structure, and support for your skin barrier along the way, progress becomes much more achievable.
If you’re feeling stuck and unsure what your skin truly needs, a professional consultation can provide clarity and a personalised plan tailored to you.
Clear skin isn’t about having the most products.
It’s about having the right plan.
If you are unsure of where to go with your skin, we offer a 10 minute phone call to chat about the best steps to get started on your journey to clear skin. Book here


 The BYONIK pulsed triggered laser is a cornerstone treatment in our skin longevity programmes.
The BYONIK pulsed triggered laser is a cornerstone treatment in our skin longevity programmes.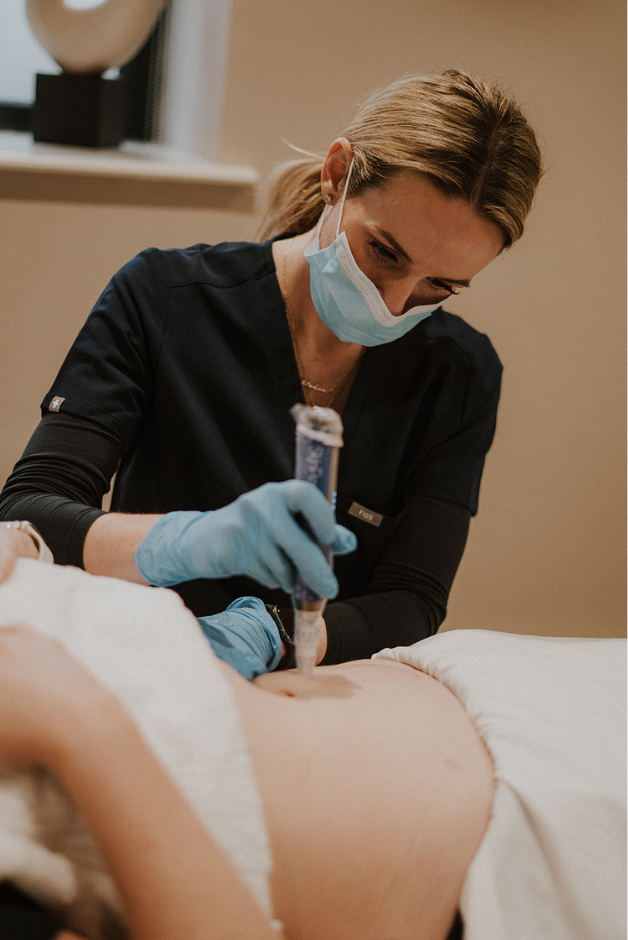 Microneedling is a clinically proven treatment for improving skin quality, firmness, and resilience when performed correctly.
Microneedling is a clinically proven treatment for improving skin quality, firmness, and resilience when performed correctly.